 
You'll also need to know when to use which drug based on each clinical situation. A basic understanding of pharmacology information includes the indications, contraindications, and methods of administration for each. It's important that you know basic information about medications and other interventions used in the PALS algorithms. Rather than merely reacting to and relying on the rhythms that are being displayed on the ECG monitor. Which is why treating the patient's symptoms, particularly when it comes to pulseless electrical activity, is so important. 
DOI: 10.1016/j.resuscitation.2018.01.041.Warning: The ECG interpretation for a patient exhibiting signs of PEA could be the same as normal sinus rhythm. "Initial electrical frequency predicts survival and neurological outcome in out of hospital cardiac arrest patients with pulseless electrical activity." C. This paper by emergency doctors from MedUni Vienna was also recognised as a "Hall of Famer" in the internationally acclaimed and popular emergency and intensive medicine blog on in March 2018 under the heading "Research and Reviews". Weiser and Spiel believe that their new findings could be incorporated into these. The international resuscitation guidelines are due to be revised again in 2020. "This enables emergency doctors to assess the situation and the patient's chances of survival more accurately and at a very early stage," say the study authors. With their recent study, the MedUni Vienna researchers have now shown that the initial electrical frequency measured by ECG is a good tool for predicting outcome and that the chances of survival are greater, the higher the still measurable heart rate. Up until now, it was thought that the prognosis for survival for PEA patients was generally poor. Pulseless electrical activity is treated by cardiopulmonary resuscitation measures such as cardiac massage and administration of adrenaline. Therefore, in contrast to ventricular fibrillation, where there is still a "shockable" heart rhythm, it cannot be treated using a defibrillator, which returns the electrical activity to an ordered rhythm, as it were. PEA means that, although the heart is showing electrical activity, this stimulation is no longer sufficient to translate into mechanical cardiac activity. "It was only when the heart rate was less and 25 bpm that the prognosis was poor (note: only a 2% chance of survival)." "Where the heart rate was more than 60 bpm, subsequent survival was 22% and hence very similar to the predicted survival of ventricular fibrillation patients (note: 30%)," explain study authors Christoph Weiser and Alexander Spiel from the Department of Emergency Medicine of MedUni Vienna. 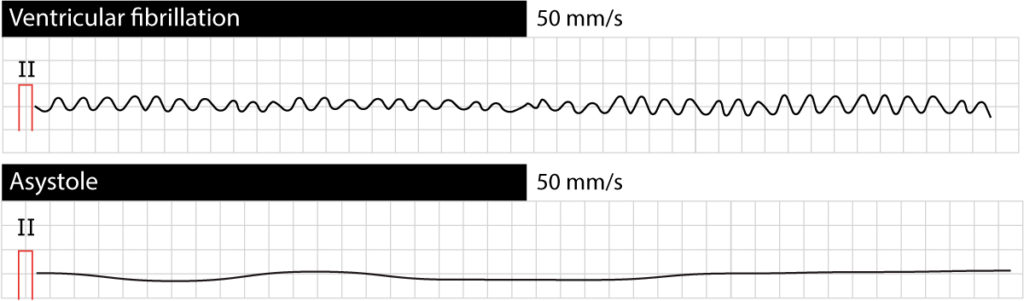
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
